Objective
The purpose of this project was to decrease the amount of skin breakdown in patients who received prone therapy after being diagnosed with severe acute respiratory distress syndrome (ARDS).
Background
ARDS is characterized by acute diffuse inflammation throughout the lungs, which causes the alveoli to fill with fluid. Research suggests that prone therapy results in a 16 percent mortality rate, compared to 32.8 percent in patients remaining supine.1 The combination of decreased oxygen saturation, hemodynamic instability, malnutrition, utilization of deep sedation, chemical paralysis, and prone therapy puts the patient at high risk for skin breakdown.
Patients with severe ARDS previously received this treatment using automated prone therapy. Due to a combination of problems – including the amount of varying stages of skin breakdown from the use of automated prone positioning in the critical care units – manual prone positioning was implemented in an attempt to remedy issues associated with automated prone therapy.
| Pros | Cons | |
|---|---|---|
| Automated Prone Therapy | • Patient proned with the push of a button • Patient, tubes, drains, and lines secured • CPR mode available | • Labor intensive (initial setup) • Difficult to assess and access patient • Increased skin breakdown and PIs • Line compression • Cost (equipment/increased PIs) |
| Manual Prone Therapy | • Easy access to patient for assessments • Decreased skin breakdown • Decrease in PIs | • Unplanned extubation • Mainstream bronchus intubation • Endotracheal tube obstruction • Prolonged CPR initiation • Labor intensive (staff) |
Implementation
An education program was developed using a literature review of evidence-based practices pertinent to prone therapy, pressure injury prevention in patients with ARDS, and device-related pressure injury prevention. The program was used to train the critical care nurses of a large urban hospital in Pittsburgh, Pa., in the safe manual proning of patients and the prevention of skin breakdown using a preventative skin care bundle. This included a turning and repositioning schedule, use of appropriately placed pillows and foam dressings, and use of a low air loss mattress. Teaching methods included video instruction, demonstration during various skills trainings, and critical care classes for new staff.
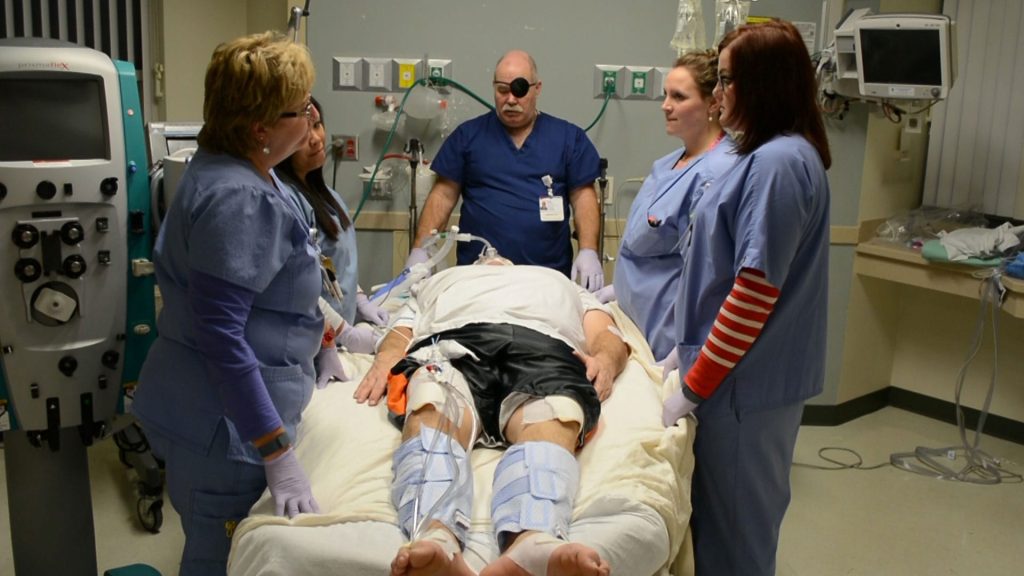
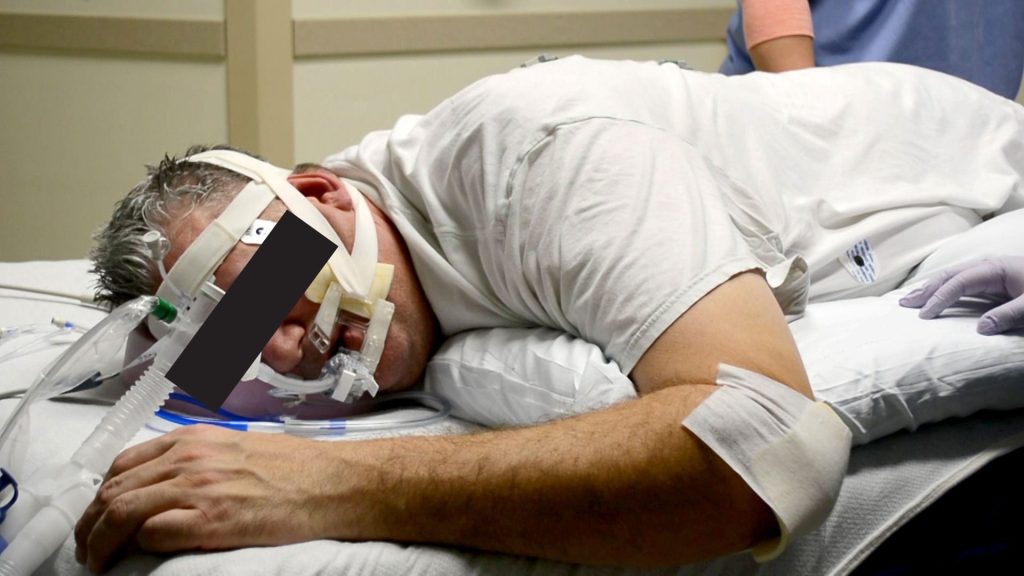
Outcome
Occurrence and severity of skin breakdown is noted to have dramatically decreased since implementation of this preventative education program. It is believed to be best practice in patients with severe ARDS.

